The most common question I get asked via comments on this blog and email is how to lower cholesterol levels and/or LDL levels. People asking this question have usually just gotten a high cholesterol reading of one kind or another and have heard the pronouncement from their doctor: You need to go on a statin.
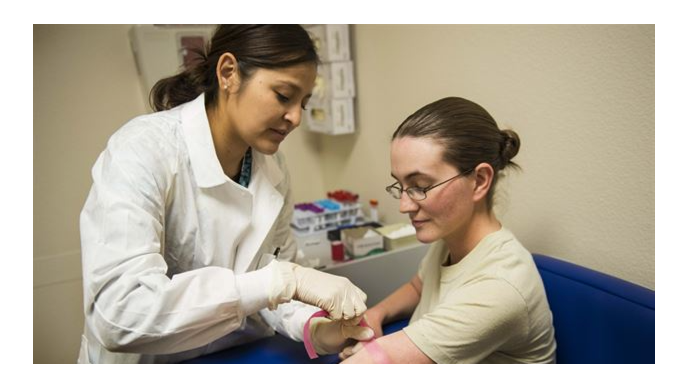
The funny thing is, most of the people asking me this question probably have read more than their own doctors have about statins. They don’t want to start taking an expensive drug with a lot of side effects and even the potential for causing death.
But, they also don’t want to confront their doctor.
They figure the best way to deal with the situation is to seek out some other way to lower their cholesterol, so their doctor will leave them alone about statins. Usually they begin by cutting the fat in their diet or more rigidly adhering to whatever diet they happen to be on. They go back to their doc a couple of months later, expecting significantly improved labs, but typically discover their cholesterol levels even higher.
There is a solution.
In case you’re not one of the people in this situation, let me give you an example of what these emails look like. Here is a message I got a few days ago from one of the few high school classmates I keep up with.
Hello Mike
Hope all is well with you. I received not great blood tests back today and my doc says has to be genetic and wants me on statin drug. Can you steer me to information about possibly a diet route? Or should I just go on statin drug – she also gave me a lab slip to check liver functions after 30 days of taking drug?! I’m looking for some alternate information. Thank you.
She attached her labwork:
- Total cholesterol 303 mg/dL
- LDL cholesterol 213 mg/dL
- HDL cholesterol 75 mg/dL
- Triglycerides 76 mg/dL
Obviously her doc was not up on the latest cholesterol news. Else she would have
- known that statins have never shown any decrease in all-cause mortality in women of any age.
- known that a higher cholesterol in a woman my friend’s age correlates with greater longevity.
- realized that a good part of my friend’s total cholesterol was made up of HDL cholesterol, which is the so-called good cholesterol.
But she was blinded by seeing the 303 total cholesterol and the 213 LDL cholesterol levels.
So, she knee jerked, said it was genetic (because my friend is a semi-vegetarian, and I’m sure her doc couldn’t fathom any other reason for her elevated cholesterol other than a genetic one, since she eats very little meat), and prescribed a statin.
There is a different solution to this problem, and it probably isn’t what you think.
I want you to take about 30 minutes to watch a video by an engineer named Dave Feldman who, using an engineering approach, has probably figured out the way for you to drop your cholesterol like a rock.
Without drugs. With dietary changes alone.
And the changes are not what you’re likely expecting.
Like Dave, I was an engineer for several years before I went to medical school, so I’m annoyed at myself for not figuring this out. But, in my defense, I came of medical age before the big cholesterol scare, and by the time it really got going, I was deep into treating patients with low-carb diets. And most of my patients saw their elevated cholesterols normalize. Not all, but most.
I always wondered about the ones who didn’t have their cholesterol levels fall (or in a few cases had them actually increase), and I watched them like a hawk. But the more people I treated and the more I studied cholesterol, the less concerned I became with elevated lab readings.
Dave Feldman came to it from a different perspective: his own extremely high cholesterol levels.
Consequently, he was highly motivated to do some self experimentation and recruit a few willing subjects (at first friends and family members) into his own study. He’s had incredible results. As have the other people who have tried his formula.
Take a look at the video, then let’s get back together below after you’ve watched it. Don’t be alarmed when the video timer says it’s 43 or so minutes long; there’s a lot of Q&A. You’ll get the meat of it in about 30 minutes. Usually I make video notes when I put up videos like this one, but I believe this one is so good, and Dave does such a great job of presenting his work, that you really need to watch to make sense of what I’ll be discussing after.
The info presented in this video is some of the most exciting work I’ve seen in a long time.
Wasn’t what you were expecting, right?
But it makes sense. Especially in view of the mechanism he lays out starting at 14 mins into the video.
A typical cholesterol experience
Let’s take a look at a well-known journalist who, despite following what she considered a perfect diet, had her cholesterol go up. This is a piece I wrote about the cholesterol trials and tribulations of Jane Brody, the health columnist (and avid high-carb, low-fatter) for the New York Times. She wrote about her experience herself, and you can find that in the link in my blog post.
You need to read this if for no other reason than that I had such fun writing it. She’s gotten her digs in on me, so I enjoyed getting a few licks back.
In a nutshell, she did what almost everyone does in this situation. She tried to be good (by which in her view meant eating low fat) and then doubled down to try to be even better. And all that happened was that her cholesterol levels went even higher.
Now you know why.
Low-carb diets and elevated cholesterol levels
After watching Dave’s video, it’s pretty easy to see why Jane Brody’s cholesterol continued to climb as she cut more and more fat from her diet. But what about people on low-carb diets? Why does their cholesterol sometimes go up. They’re eating more fat, not less.
I’ve got a news flash for you.
Despite being hash tagged as #LCHF (which if you don’t know, means Low-Carb, High-Fat), low-carb diets are, for the most part, low-fat diets.
Say what?
There are two ways of looking at fat. One way of measuring the fat in the diet – and this is the way most people look at it – is as a percentage of calories. In this way of calculating, if half your calories are fat, then you’re on a 50 percent fat diet.
Another way is to measure the actual amount of fat you eat irrespective of how it compares to the total number of calories you eat. This is the way your body does it. Your body doesn’t care what the percentage of fat is – your body wants to know how much fat you’re eating. How many grams. Is it enough? Is it too much?
The whole percent calories deal is a nutritionist construct for who knows what reason. It’s immaterial other than to those who want to flog you for eating too much fat.
Let me show you what I mean.
I don’t want to go through all the calculations for an entire day’s worth of food on a Standard American Diet (SAD) and a low-carb diet (or #LCHF, if you prefer), so I’m going to use a typical lunch as the proxy for an entire day.

If you’re on the SAD and you waltz into a McDonald’s for a quick lunch, you may end up with a Big Mac, an order of fries, and (I’m giving the SAD a break here because odds are it would be a supersized sugar-sweetened soda) an unsweetened ice tea. If you go to to the USDA National Nutritional Database, search for these items, and figure out the calories, fats and carbs, you’ll come up with the following numbers:
- Total calories = 941
- Fat calories = 459
- Carb calories =376
Fat calories = 49% of calories.
Which is much higher than the 30% to 35% fat most nutritionists recommend. To them, 49% of calories is a lot of fat.
(Worth noting that the meal would be lower in percent fat if we’d added in the sugar/corn syrup calories of a supersized soda, which by itself could top 400 calories! That would have dropped the meal to 34% fat and all the nutritionists would have doubtlessly applauded.)
Now, let’s go through our low-carb dieter’s selection. Our LCHF hero orders the Big Mac without the fries. And has the unsweetened iced tea. He — or she — then gets rid of the Big Mac bun and scrapes off as much of the Big Mac sauce as possible, because it’s filled with added carbs and nasty vegetable oils. This #LCHF meal ends up sporting the numbers below:
- Total calories = 350
- Fat calories = 234
- Carb calories = 60
Fat calories = 67% of calories.
Call an ambulance! Immediately! Heart attack waiting to happen. Fat at 67% of calories is more than double the amount most nutritional experts would recommend.
But wait.
There’s more to the story.
I didn’t show the actual amount of fat in the first ‘regular’ Big Mac lunch, nor did I show it in the #LCHF version.
So let’s take a look.
The regular Big Mac lunch with all the sauce and the fries contains 51 grams of fat.
The #LCHF version (emphasis on the High Fat) contains a mere 26 grams of fat, just about half the fat of the regular Big Mac meal.
Most low-carb diets are like this. They are really lower-fat diets when compared to the SAD.
And they are lower-calorie diets as well. Compare the calories in the full Big Mac meal to the #LCHF version. Way less than half.
So, if, as Dave Feldman’s data show, eating fat is what makes your cholesterol levels go down, you can see how going on a low-carb diet could end up making your cholesterol go up. And it’s easy to see the fix, oui?
Since I’ve used the example above, I’ve got to digress for a bit to tell you something that always slays me.
Have you ever noticed that if you go out to lunch with friends and have the Big Mac meal with fries and everything, no one really says anything to you? But if you don’t order the fries, and you throw away the bun, and eat only the patties and the little lettuce, tomato, and whatever comes with it, people say: “Oh, you’re on one of those crazy low-carb diets. Don’t you know those will wreck your kidneys, and all that fat will clog your arteries?”
I can’t tell you how many times I’ve heard it. It’s fewer actual grams of fat, but now suddenly because it doesn’t contain the added starch of the bun and the sugar of the sauce, it’s a dangerous high fat diet.
Okay, digression over.
LDL particle number
The LDL particle number (LDL-P), as contrasted with the LDL cholesterol level (LDL-C), is maybe a term some of you aren’t familiar with.
Since the medical mainstream, especially that part of it that makes statin drugs, but also the part that promotes them, is so convinced that cholesterol is the driving force behind heart disease, they keep looking for more and more ways to slice and dice cholesterol.
I’m not sure, but it’s probably all in an effort to find the Holy Grail of cholesterol measurements, the one that absolutely correlates with heart disease, and is finally found to be causal. They haven’t found it yet, but they keep trying.
One of these numbers is simply the number of LDL particles in a given volume of blood.
If you divide the LDL-C level by the number of particles in the sample, you can determine the size of the particle. Generally, the larger the LDL particles, the better. So, if you don’t have a lot of LDL particles and you have an average amount of LDL-C, then dividing them as described results in your having large LDL particle size.
The proponents of the low-fat diet crow that they lower LDL-C. And that’s generally true. However, one of the problems with the high-carb, low-fat diet is that they also tend shrink LDL-particle size, which is not a good thing.
Their LDL-C goes down (but not always – see Jane Brody’s case above), while their particle number stays the same, resulting in smaller, denser LDL particles. A bad thing.
Some lipidologists now consider LDL particle number to be the most important measurement, so it’s another nail in the low fat diet coffin. And it’s reassuring to know that Dave Feldman’s data show that consuming extra fat decreases not only the total cholesterol and LDL-C but the LDL particle number as well.
Does the Feldman approach work with the Standard American Diet as well as it does with the ketogenic diet?
We don’t know. He’s tested it only with the baseline being the ketogenic diet. And, there is no data that I know of showing what would happen were you just to go face down in the extra fat while eating the SAD.
There are some old studies out there kicking around showing that people who fast actually drive their cholesterol levels up, which goes along with Dave’s theory as to mechanism.
During a fast, the liver is sensing no fat coming in, so it jumps into action to package some and send it to the tissues.
But no real studies I’ve seen examine what happens when you add the extra fat to the SAD. (As of this writing, I can say there may be such studies, but I’m in a plane somewhere over the Atlantic as I write this and can’t search for them right now.)
Dave keeps up with all this on his site cholesterolcode.com, so I would encourage you to go there and look at the data. He posts new data there all the time.
If you do try this on your own and do the Feldman protocol, be sure to send your results along to Dave to add to his rapidly growing database.
And keep me posted as well. I would love to hear your experience.
In case you’re interested, I had my own cholesterol checked a couple of years ago, and here are my numbers. I suspect they reflect the low-fat, low-calorie nature of my regular #LCHF diet. I’m going to load up on fat before my next labs to see what happens. But I already have a pretty good idea.
Based on Dave’s work, if you add more good saturated fat (on a low carb diet) even in just the few days before a blood test, the lipid numbers will likely look ‘better’, whatever that means.
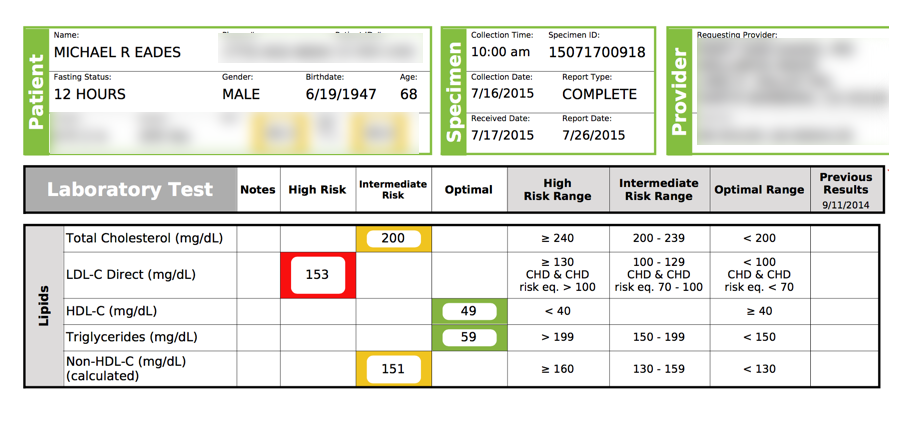 Cholesterol, fat, and statins
Cholesterol, fat, and statins
The take home message I want to leave you with is how rapidly changeable cholesterol values can be.
Dave Feldman’s data has shown that eating fat three days before can markedly alter your total and LDL cholesterol numbers. Eating fat five days before can bring about huge changes in your LDL particle number.
Given that cholesterol levels and particle numbers can change dramatically in just a matter of a few days, why in God’s name would anyone want to go on a statin because of a single ‘snapshot in time’ cholesterol reading that is a little high?
Depending upon what you eat, it may drop like a rock in a couple of days.
Statins are not benign drugs. They come with a host of side effects, occasionally fatal ones.
You end up having to have your liver monitored closely, which requires extra trips to the doctor’s office, which are expensive, and extra sticks, which are painful.
And that doesn’t include the expense of the drugs.
Additionally, you risk developing diabetes (females in particular), muscle aches and pains, and memory loss. Plus, at this stage, no one knows what the long-term overall effects are on cholesterol-dependent tissues, such as the brain.
And it horrifies me to think how many people are taking them right now based on just one single cholesterol reading that was a little high.
The statin decision is a choice you’ll have to make along with your physician. I just think you need to have all the facts at hand before you even consider taking the statin plunge.

Hi Dr Mike – that was really interesting. I’m on a LCHF diet. I’m not low calorie at all (three cooked meals a day with substantial snacks inbetween – I’m still too lean) but I don’t know if I am ketogenic – I get 30 to 50g carbs from green veggies, milk (full fat) in tea and coffee, almonds and a glass of red wine with dinner. I have quite a lot of protein because I like protein foods as in oily fish and red meat and eggs, but I add coconut oil if the meat is not fatty, also add coconut oil to the all the veggies as I sauté them (three times a day), and cook the eggs in coconut oil. I wouldn’t know how to exactly evaluate how much fat I’m getting though. I’ve been tracking my lipid profile, which my GP tests every six months, for the past ten years. It rose exactly after adopting LCHF, rose steadily from bog standard year by year. I don’t mind, just the GP does as it’s so high – though HDL very high (135) and trigs very low (44) so he’s okay about the profile. I’d like to lower the LDL while raising the HDL even higher ! I wonder if I need to cut the protein and raise the fat, not sure how to raise the fat really, other than adding even more coconut oil !
You could add Macadamia nuts. They are an easy way to increase fat intake. If you’re happy with you diet as it is, and you would just be doing this to assuage your GP, I would just load up on the extra fat starting three days before your next lab test. Then follow your regular diet the rest of the time.
Yes I’m happy with my diet as it is – I will try the loading three days before the next test like Dave Feldman. Not with 5,000 calories though, I could never physically eat that quantity of food, even if it were mostly comprised of fat !
Hi Anne–
From the numbers you cite, you fit the profile of what I call a Lean Mass Hyper-responder (LDL above 200, HDL above 80, TG below 70). You might want to take a look at the article I wrote on this given how commonly I’m seeing this profile with lean and/or athletic low carbers. http://cholesterolcode.com/are-you-a-lean-mass-hyper-responder/
Hi Dave,
I actually looked at that article just yesterday, before I read your reply above, and thought that might be me ! I also do Slow Burn/Super Slow weight lifting three times a week (been doing that the past ten years so quite heavy weights now, especially considering I’m 64), and I I walk 5 to 6 miles per day.
Do you think eating more fat the three days before the next cholesterol test (September) will lower the total and LDL in a “lean” hyper-responder ? I find it difficult to eat more fat than I already do, adding it to everything !
Not that I’m worried about my cholesterol levels, but I found what you have discovered extremely interesting.
Isn’t it interesting too that lipid levels are so variable – makes a nonsense of the test.
Yes, Anne, I do think it is probable that an increase in dietary fat for the 3 days before your test would likely lower your total and LDL cholesterol.
That said, I may have a *new* solution in the works soon based on my most recent experiments. But I’m verifying these patterns on myself first before going public with them.
And yes, the bigger takeaway is this entire lipid system is *far* more dynamic than is currently believed. Taking a single, annual cholesterol test and it resulting in a lifetime of medical therapy without considering this simple reality seems completely insane to me now. Even if one didn’t believe in LCHF, I’d want them to at least know just how much these numbers are impacted by what they ate in just days before their test.
Hi Dave – If you consumed the amount of extra high fat you take in the three days before your cholesterol test for several weeks or months (or longer), do you think your total and LDL still be as low as it changes to when you only increase it for the three days before the test ? Or is it the sudden increase in fats, so to speak, that affects the results ?
I’d speculate the former, but I haven’t done a long running enough test to find out.
It works ! It works !! I eat high fat/low carb, have done for about ten years, but for a week before my lipid test last week I ate extra, extra high fat. My total cholesterol came down from 8.7 (336) to 5.5 (212), my HDL remained exactly the same at 3.5 (135), my triglycerides lowered from 0.5 (44) to 0.3 (26), and my LDL lowered from 5 (193) to 1.8 (69) !
I’m in France at the moment so can’t get online easily but managed to post this as I couldn’t wait to let you know.
I’m very lean btw.
Hi Dr Mike – can you let Dave know my good results of taking the extra high fat please as I know this is an ‘old’ thread, au revoir, Anne
Will do. Glad you did so well.
Anne–I’m curious how many calories you ate for the three days and what foods you added to raise up fats, but keep carbs low.
Hi B. Johnson – sorry for the late reply, I’ve been away and only just got back.
I’ve no idea how many calories I ate, I don’t count calories, I only count carbs. The foods I added to raise my fat intake were increased amounts of coconut oil, some cheese (which I don’t normally eat as I eat Paleo) and the addition of macadamia nut butter. I ate my usual three meals a day consisting of meat or fish with green veggies sautéd in coconut oil, then also about five high fat snacks of the macadamia nut butter and cheese. The only carbs are those in the green veggies, which is practically nothing, and some milk in tea and coffee, plus one glass of red wine a day. I didn’t put on any weight – I stayed as lean as I always am. I was very surprised I must say, Anne
I had sleeve surgery 2 years ago. Is a lchf an option for me?
No reason why not. With portion control so as not to overwhelm the volume that’s comfortable.
Every time I go in, my doctor wants me to take a statin, which I refuse to do. Here’s one solution: don’t have the prescription filled and don’t take the statin, end of story. But in general, I simply say “I’m not going to take a statin” and that’s the end of the discussion–apparently, based on the way I say this, my doctor can tell it’s futile to argue with me.
Most people don’t have your fortitude when confronting their doctor.
I said exactly the same thing to my doctor. She doesn’t even mention the word statin when I see her now. My total cholesterol is 600, LDL 500, HDL 98, Trig 98. My NMR tests showed all very large pattern A particles.
Thank you!
You’ve provided a lot of wonderful information for years, and this is right up there near the top. A great service to us all.
Hi Mike – so happy to see you back writing these columns – and this was the best yet! Can’t wait to send it to my husband – and hundreds of friends.
One typo – “Know you know why.” It’s right after the para on Jane Brody.
Cheers,
Marcia
Fixed it. Thanks.
“So, if, as Dave Feldman’s data show, eating fat is what makes your cholesterol levels go down, you can see how going on a low-carb diet could end up making your cholesterol go up.”
Did you mean a low-fat diet like Jane Brody was on?
No, I meant a low-carb diet. I was using the Big Mac example to show how fat intake could actually go down on a low-carb diet. If it does go down, according to Dave’s data, your cholesterol reading could go up.
OK. But not everyone who goes LC comes to it from a burgers’n’fries lifestyle. Many people probably come from the low-fat diet their doctors recommended.
It would be interesting to ask people who complain that their lipids increased on a LC diet what they were eating before.
While I didn’t have time to get too deep into it within the video, it’s worth emphasizing that many (like myself), will see their “baseline” cholesterol go higher after starting a low carb diet. Thus, the Inversion Pattern is what modifies it from there.
There’s a key part in the video where I do a grand overture to how a Low Density Lipoprotein’s *PRIMARY* job is to distribute energy from fat. I do this because when we are powered by fat, the body has a very good reason to circulate more LDL particles given they are providing the triglycerides (3 fatty acids) to our cells for fuel. Cholesterol “ride shares” with this energy in the same boat, which is why it makes sense for it to increase in a blood test for someone who is on a low carb diet.
But again, as I say in the video, most LDL triglycerides will get dropped off to cells. Whereas the vast majority of LDL cholesterol just rounds its way back to the liver to be reused for many other fates. It’s more like the backup medicine in case cells need to uptake it for medicine/repair (endocytosis).
I came from a very low fat/high carb diet to a ketogenic/zero carb (meat/eggs only) diet 2.5 years ago. My total cholesterol shot up to about 250 (LDL 150, HDL 85, Trig 55) at 9 months into it. By 20 months into zero carb, my total cholesterol shot up again to 600 (LDL 500, HDL 98, Trig 98). I’m eating WAY more fat than I was eating on my previous low fat regimine. My total daily fat intake now is around 70-100 grams.
Gretchen—the point he was making is that you might eat a larger percentage of fat and a lower percentage of carbs and protein on a LC diet, but if you eat less food overall, you could actually be consuming less fat than previously.
In the example, you threw away the bun, fries and sauce, eliminating lots of unhealty fat and carbs from your meal. However, since you didn’t replace those items, you ended up eating less fat than before, even if that fat is now a higher percentage of what’s left.
If you eat just the burger patty, that will be less total fat than the patty + bun + fries + sauce (we’re ignoring that those are unhealthy and just looking at the total). That was the point of the illustration—you can eat a high-fat diet and still eat less total fat than someone eating a standard diet.
As always Dr Eades, this is absolutely brilliant. Thanks for sharing. I have a close friend who has been penalised on her life policy because of a slightly elevated cholesterol score. Can’t wait for her to see this.
Thank you Paul – that makes it very clear.
Thanks for the interesting post. Now I will start looking more closely at the composition of my diet, although my cholesterol was “good” last time.
When I was a young surgeon, busy private practitioners ruled the roost and could cower a hospital administrator. The internest with the largest practice in our hospital was a flamboyant fellow who made rounds with the charge nurse pushing a cart loaded with charts. He bragged about being among first to recognize the importance of cholesterol and heart disease. How things have changed.
I wonder if he’s still bragging.
I can verify that fasting raises your “cholesterol”. I made the mistake of having a blood test taken after 4.5 days of fasting, and my doctor freaked. I subsequently got two tests: the first taken after 12 hours of fasting, on Monday; the second taken after 4.5 days of fasting, on Friday of the same week. Went up: total cholesterol, LDL, triglycerides, non-HDL cholesterol. Went down: HDL, blood sugar. I did not pay for the extra LDL-p test, only for the Friday test (Monday’s test was normal doctor’s test, which does not include anything fancy; I paid myself for the test on Friday.) So, I don’t know what LDL-p does. I do know that I have four tests of LDL-p, two taken after 4 days of fasting and two after normal 12 hours fasting, and the two taken after 4 days of fasting are much higher than the two taken normally. However, there were months between these tests.
I have not tested Dave’s theory of eating more fat for three days before a cholesterol test, though I will. I saw his presentation at Ketofest in CT, and thought it was great. I will use a similar protocol to what Dave used, where I take one test, fast for 3+ days, take another test, eat high (animal) fat for 3 days, fast 12 hours (overnight), take another test. I’ll send the results to Dave.
Let me know what happens, too.
If you haven’t already, you should check out my own recent experiment of fasting for only 2.5 days (spoiler: highest LDL score I’ve ever had!) http://cholesterolcode.com/the-fasting-disaster/
I am a retired orthopedist. I got away with the statin problem by writing my doctor ( a great guy and excellent physician) a letter to be placed in my medical record notifying him that for personal reasons I would refuse taking statins and that I understood that according to current guidelines he had to offer them to me. That covered his butt, kept me off statins and we are still good friends. Let’s not forget that big Pharma has made it very hard legally for docs to use common sense if it goes against their profits.
Probably something every one should do.
Thanks Doc!
blood test tomorrow to get my GP off my back. I’m going to load up on saturated fat the rest of today!
Don’t know if just the day before will help or not. I’d give it a try though.
When Dave gave his presentation at KetoFest, he said it took three days. Not sure what one day would do.
I get plenty of saturated fat in my diet. When we have steaks or chops my wife and son cut around the fat. Since reading the 6 week cure I eat what they cut away off their plate. Normally the day before a blood test I would lay off. Today I’ll go heavy instead!
Lemme know what happens.
will do
Doc,
got the call. Much improved. I’m picking up the numbers this afternoon and will send you an email with the exact improvements.
Thanks for empowering us!!
Thanks in advance. I’ll be eager to see your results.
sent the email. Thanks again!!
Thanks for posting this. Although I’m not at all concerned about cholesterol, my doctor insisted on a cholesterol test a couple of years ago. My results came back higher than the lab thought they should be, although my triglycerides were very low and my HDL was quite high. The doctor’s office followed up with the usual recommendation to eat less saturated fat, which I ignored. Now I’ll be prepared the next time I’m facing a cholesterol test. I’ll load up on fat and wow them with my results.
Scarecrow: But that’s so easy! I should’ve thought of it for you –
Tin Man: I should have felt it in my heart –
Phil
I found this paper a few years ago
Benefits of High Cholesterol by Uffe Ravnkov MD PhD
You will need to google the title to find it.
I have a 10 page pdf file if you are interested.
Email me at chuck5620@gmail.com and I’ll send you a copy.
A good read!
Another myth bites the dust!
Chuck
I emailed you. Thanks in advance.
I actually used another of Dave Feldman’s hacks to lower my LDL–but you probably would not approve. I have been eating very low carb (<20g) for over a decade, and even though I've had a VAP test that showed my LDL to be 100% pattern A (large, fluffy), my doctors still made noises about my LDL, despite high HDL (90s) and low trigs (<50). I've ignored them but decided to experiment with one of Dave's suggestions. I get labs every 4 months (hypothyroid).
For 3 days prior to my blood draw, I ate very low fat, higher carbs (c. 150g daily). No junk–just beans, brown rice, veggies. I was amazed at the results. My HDL remained high, my trigs were low, but my LDL went down 45 points! My endo commented on how well I did, and in the interests of full disclosure, I explained my dietary 'hack.' I added that it reminded me of how I had to eat carbs prior to my GTT a few years ago, so perhaps this isn't distorting my LDL, it's more accurate.
My endo admitted that was logical, but he was not concerned at all about what I'd done to get the number. I had absolutely no problems other than the increase in appetite by the third day, but after the blood draw, I went immediately back to my low-carb eating.
I approve of anything that gets your doc off your back about your cholesterol levels.
I’m doing that with red rice yeast and niacinamide. I did that in 2011 with my previous doctor (- the red rice yeast but with lecithin). Levels dropped 30 points within 30 days and he wasn’t impressed. Still wanted me to take a statin. I refused. Then he tried to talk to me about an Rx for a time release niacin from one of the drug companies. I told him the niacinamide, which he just said didn’t impress him but wanted to Rx me niacin, was $6 at the Vitamin Shoppe. I never saw him again.
Funny thing, he now runs a weight loss clinic prescribing shakes and bars.
Could it be that Emmie is hypothyroid because of <20 carbs per day for over a decade!?! Dr. Atkins warned against being very LC for so long.
No, I am not hypothyroid because of low carb eating. I have Hashimoto’s (autoimmune disease) and have been hypo for many, many years–before eating very low carb.
In fact, my endo thinks my low carb diet is superb.
I now understand why so many people have cholesterol readings that get them an rx for statins! How many people are told to go for blood work and being totally afraid of what the results will be, spend a week or more “being good” before the blood is drawn. Which means eating all the stupid things we’ve been lectured about for years; extremely low fat–especially saturated fat– and high carbs, especially those “healthy whole grains”! The test comes back and, of course, is a disaster. These people, had they continued eating the fats and lower carbs they normally do the week before the test, would have had better results! I gave up all grains and sugars as well as vegetable oils in May of 2014. Despite the fact that I feel better than ever (I am 67 years old) and have lost 170 pounds (the last time I weighed was in March), everyone feels it is their duty to constantly lecture me on the evils of eating Keto. I hear about how all that fat is busy clogging my arteries, destroying my kidneys and is going to kill me! Giving them the facts does no good, so I simply say, “Well, if it does kill me, at least I’ll feel GREAT when I die!!! Having weighed 400 pounds when I graduated from high school in 1968, and spent most of my life at that weight, I now weigh 230–would like to lose another 40 to 50 pounds and feel it is the high fat low carb intake that made it possible. I therefore don’t worry about cholesterol or fat intake and just “keep on keepin’ on”! I wish everyone could be REQUIRED to read this blog and watch this video! Thanks Dr. Mike!
Great job! Not many people do what you’ve done. Congrats on your success!
“If it does kill me, at least I’ll feel GREAT when I die!!!”
I’m gonna borrow that!
Fabulous. Love this so much. You do you!
I’ve been doing LC for about 5-6 years and never worried about how much healthy fat I got . . . always HIGH. 2 years ago I was diagnosed with congestive heart failure from a congenital defect in my atrial valve. My husband and (almost a nurse) son sat in on the angiogram and my arteries were clean, slick as a whistle!!! They gave me a TAVR to fix the valve and the surgeon ordered a “heart healthy diet” for me in both hospital and rehab. I tell people that he nearly killed me again! After a month on that diet I was once more addicted to all the carbs, but I got back on keto, lost the gained weight and am doing great! I refuse ALL meds and treat myself with natural supplements.
Rick — that’s exactly right! I’ve had so many people write to me on this very issue and it genuinely breaks my heart. In anticipation of a terrible score, they do what *intuitively* makes sense: lower fat or fast altogether — not realizing they are spiking their score dramatically.
This is especially hard for low carbers as they often feel “everything else is right” with their bodies and their bloodwork.
Brilliant as always, Mike
Thanks, Jonny.
What is implicit in Feldman’s work is that every trial ever carried out with respect to statin effects on cholesterol profiles was complete, and total rubbish. If the drug companies had accounted for the timing and amount of macro nutrients consumed before the measurement of cholesterol they would have realized that they did not have a product.
Just for laughs my doctor gave me a handout that stated that I should eat foods containing less cholesterol. And this is the Kaiser Health Foundation, that surprisingly has next to nothing to do with my health or anybody else’s, the exception being acute care.
That’s exactly right! I brought this up in my most recent presentation and stated plainly, “Look, if the experiment didn’t tightly control for each subject’s diet in the three days before each blood test, then I can’t trust it.” And of course, I don’t actually know of any that have.
Hi Doc
Great post!
As stated above, high cholesterol is often attributed to genetics by doctors when there is no apparent reason for the elevated reading.
Could you clarify if there is a difference between high cholesterol and familial hypercholesterolemia (FH). I thought FH was a genuine genetic condition. I thought the high cholesterol readings in your blog weren’t too high compared to mine: my average is 11.9 mmol/L (x 38.67 = 460.17 mg/dl) with a record high of 18.4 mmol/L or 711.53 mg/dl).
I even have xanthelasma (cholesterol in the knuckles)!
So, does the above apply? I’m a bit confused and not a medical man/scientist.
Off topic – I’ve just read Prussian Blue – the latest Bernie Gunther – I seem to recall you recommending him a few years back. Another fantastic Bernie Gunther novel!
Regards
Charles Gale
Yes, familial hypercholesterolemia is different and is genetic. I’m not sure how Dave Feldman’s protocol would work with FH as I don’t know if he has data on this or not.
Hah! Funny. I just finished Prussian Blue a couple of days ago. It was one of the books I took on my recent European trip. Great book, as are all the Bernie Gunther books.
Most FH diagnoses are done without genetic testing. It’s just assumed that if your LDL is elevated and you have xanthelasma, you’ve got it and you should stop thinking critically and just go face down in statins and PCSK9 inhibitors. But even putting aside whether the medications even make sense for FH patients, finding out whether you’ve really got a genetic situation, and figuring out exactly which genetic tests to take to confirm it, is not straight-forward.
I would like to see these results matched with adipose hormone profiles taken at the same times. That would really add to the narrative. I am aware of doctors’ efforts to prescribe statins, and have politely avoided having to comply so far.
“You end up having to have your liver monitored closely, which requires extra trips to the doctors. Which are expensive.”
There you have it.
Interesting. Thank you for this.
Over the past four years, my own experience has been that averaging around 75 grams of carbs a day; using no added fats except butter, unadulterated heavy cream, and coconut oil, in a range — with the meat I eat — of about 155 grams of fat a day has kept my HDL in the 80s, my triglycerides and A1C well within range, and my total cholestrol downward trending from 257 to the latest number of 230. So, even with a more moderate low-carb-high-fat program, at least one person has had good results.
Most people do have good results with the low-carb, high-fat diet, but for the ones who don’t, I expect it’s that their fat intake isn’t high enough to drop their cholesterol levels. In your case, it it ain’t broke, don’t try to fix it.
Here’s a story about how the medical community is misusing statins. My husband had a severe bout of vertigo a couple years ago. We weren’t sure if it was that or maybe a heart attack or stroke, so off to the ER we went. They did an MRI and CT scan and admitted him overnight for observation. When the doc came by to see him, he told him they were giving him a statin. I asked him why he was being given a statin when stroke had been ruled out and his bloodwork was NORMAL. He said it was because he had originally been admitted under suspicion of stroke and was thus on “stroke protocol”. Just stupid. I sort of read him the riot act over it and told him my husband wasn’t taking any statin, and he absolutely did not know how to respond, unless the partial eye-roll and “sheesh!” attitude count. He eventually said that my husband was a grown man and didn’t have to take it if he didn’t want to. My question was what sense did it make to prescribe it in the first place?
To further illustrate the general mishandling of his complaint, no one tried any canalith repositioning maneuvers to see if it was just plain old vertigo. It would have taken about 90 seconds. I read about them later when he had another attack, tried one on him, and it worked like a charm, instantly. And it didn’t cost us $13,000 either.
My own experience with low fat, high cholesterol is in line with Dave Feldman’s research: in 1990, I was a 29 year old vegetarian with an aversion to eggs and had very high cholesterol; my doctor said “you just don’t see it that high in a woman your age”. He told me I had no reason to ever eat eggs. No problem. He also said I might have to go on a statin. I couldn’t afford it at the time, thank goodness. I now eat mainly LCHF, loads of eggs, beef, butter, etc., and while my cholesterol is a bit higher that what the industry likes to see, my ratios are generally good enough to not concern my (enlightened) doctor too much, though I would like to see improvement in HDL. Maybe tightening up on my LCHF diet some will get me there. Thanks for this posting, informative as always.
Thanks for the interesting history. It always amazes me how tied to statins so many docs are.
Thank you for your continuing education for lay people like me.
What are the best fats to have? I am wondering how to increase the fat that I am intaking?
Thank you.
One source would be Macadamia nuts. Other than the Macadamia nuts, try to stick to foods of animal origin.
I’m not necessarily recommending people up their consumption of fat, because it can interfere with weight loss, if that’s the goal. The increased fat is a hack to get cholesterol levels down to make your doctor happy.
Thanks for this information. I am a 73 year old female with chronic high cholesterol.
Total Chol. 394, Tri 167, HDL 56, LDL 305. Of course my MD wants me on statins, which I have refused. For the past 1 1/2 yrs I have been on LCHF diet and reversed my diabetes, lost 22 lbs and from then on for the next year I have not been able to loose any weight. I just don’t know what to do and don’t know where to turn. I know this diet works…my husband has lost 20 lbs. If you have any advise I would appreciate it. thanks for letting me vent.
I can’t really give medical advice over the internet. But I can tell you that in people your husband’s age, a higher cholesterol level correlates with greater longevity.
My goodness, my head is reeling! BRILLIANT!
But now for the $64,000 question. How much fat (and saturated fat) constitutes a TRULY high-fat diet? I’m female, 5’6″ and currently weigh 190. Just how high would I have to go to ensure a good test … along with the health and vitality that a keto diet is sure to give me?
Might 150 grams of fat be sufficient? More?
I haven’t had a cholesterol panel done since 2009, and I’m thinking he’s going to ask for one when I have my physical on Friday.
According to Dave’s date, you’ve got to crank it up pretty high. I would think 150 gm extra should do it. But time it properly according to what he says to get the maximum benefit in terms of cholesterol lowering.
But remember, this isn’t going to help you lose weight. Adding fat will halt your weight loss, so you’ve got to decide what you want to do.
Yes, understood. My physical is tomorrow, and I just found out they draw the blood right there (never used to). Since I haven’t been taking in that much fat, I’m going to beg off and offer to do it later. After the draw, I’ll go back to eating a more moderate amount of fat. My losses have started again. I’m 10 pounds less than I was at the beginning July, so it’s a start.
Thanks for the response!
Your article and video gives me some reassurance that my low carb diet is not futile or harmful. I thought my numbers were high (TC-170,TG-45,HDL-63), but his are through the roof.
1) What concerns me are the articles that suggest a high fat diet(HFD) like the SAD will increase prostate size and maybe even cause prostate cancer. That really worries me. They say the HFD causes low level inflammation. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4583131/
2) Funny enough, since I started eating 2-3 baked potatoes a week, my leg cramps in my thighs have completely gone, but I still get them in my left ankle top. (And I get plenty of salt)
3) Nobody says much about sleep problems on keto diet, but plenty of people mention it.
My doctor will not let me get an NMR. I have asked a few times, but he says it isn’t necessary.
but he says I really need a statin
I meant TC-270
Hi Dr Mike, very interesting video. Just wish I could benefit from it. I am so discouraged by hearing all this because I seem to be a true outlier. I’m 64 yrs old now and have had my cholesterol numbers checked many times over my lifetime. Total C has always been higher than my Dr wanted. I have gone on extended experiments of N=1 to see how it changed. Always, without fail, my TC and LDL go up very high when I eat a saturated fat diet. I have followed a protocol very similar to the one in this video which I devised myself many years ago to see if I could affect the numbers. I lived a strict paleo LCHF life for several years and my numbers continued to climb (last reading TC=377, LDL=227, Trig=88, HDL=75. A couple years ago I decided to do an Ornish type diet, and was very strict, no fat at all, and only complex carbs for two weeks. My TC dropped from 357 to 206, LDL from 180 to 14o and Trig from 82 to 106. I don’t know what to believe. I have always felt healthy but just a few months ago my fastin glucose went from 79 (same all those years) to 93 and more worrisome, blood pressure is now in the 140-150 range when it was always around 100-110 before. Don’t know if BP is related to all this lipid stuff, but I am getting very concerned and absolutely don’t know what to eat anymore!!! Wish I could get someone to help me figure it out. Sorry but this video only got me more confused. Any help is greatly appreciated.
If you eat what the old food pyramid recommended and are adding more fats, it may drive up your cholesterol. The idea is to lower your carb intake. Cut all sugar, all processed foods, all starches including pasta and rice. But add more fat to replace the carbs you are cutting and so you aren’t sending starvation signals to the brain. Add in coconut oil, avocado oil or avocado, olive oil, organic butter (such as Kerrygold) and heavy whipping cream. Eat more non-starchy veggies.
And don’t worry too much about your readings. I have really high numbers. My cholesterol is around 700+, triglicerides are in the thousands and my hdl is 38. I’m actually doing better than I was at the beginning of the year when my numbers were worse. I was trying to cut carbs without adding enough fat. Now I’m adding fat and am much stricter with the starchy carbs. I also have fatty liver, but I’ve been reading that losing weight overall can improve fatty liver. As I watch the video Dr. Eades included above, I realized that blood tests recording cholesteral are completely useless as the numbers can improve drastically and go belly up just as fast, depending what you have eaten in the previous few days. So it can be an entirely different reading within days. This means that the test of one or two days a year does not tell you anything about your cholesterol except what you’ve eaten in the past few days before the blood draw.
And as far as statins, that was the first recommendation my gp made. I gave it a try but it was only a few weeks later I would be getting stiff sore forearms and pain trying to go up and down stairs. So I quit and said why and the doc didn’t put up much of a fight. Her parting remark was that I was probably only still alive because of my sense of humor.
You’re blood sugar levels are pretty low. I have diabetes 2, so my numbers are only low when I am strict about no sugar and no starch. And that means I try to keep my blood sugar under 110.
Sharla
Sounds like you should split the difference: not too low carb, but not too low fat either.
Maybe iodine deficiency , carb deficiency, or T3 too low?
http://perfecthealthdiet.com/category/biomarkers/hdlldlcholesterol/
The Book Deep Nutrition says to limit sugar and bad fats. see chapters 8&9
I didn’t know the bad fats were that dangerous. vegetable oil other than olive oil and fried foods. sounds like fried foods mess up endothelial function. there is a picture on page 277 you might find interesting
Gary Taubes book GCBC has a chart of cholesterol to mortality and the elbow of the curve is around 250 TC. In other words, not anything too worry about until well over 250 or higher? maybe? Who knows?
get that BP down
BTW, I stopped decaf, real coffee, tea and chocolate and my leg cramps subsided greatly. Dr Superko I think mentions that decaf raises LDL
http://www.medscape.com/viewarticle/788017
Reading the book “Mastering Leptin” might prove beneficial. give it a try
Great post! Wondering how much fat one needs to load up onto get results or if it’s necessary to eat 5000 calories for 5 days. That can’t be easy. And if the quantity required is. different for a man or woman
All very interesting, and statins should not be prescribed unless one has CVD which biomarkers may or may not indicate; but of course a calcium scan does, so if family history an issue with high LDL-C or P, Doc should have the patient get a scan; if that is positive then seems to me a statin may make sense; your view?
What level and kinds of carbs do you consume to have such a good TRG score?
Had not thought about low carb being low fat as you pointed out; quite insightful !
I usually keep my carbs in the 50-100 gm/day range.
Great post! Wondering how much fat one needs to load up onto get results or if it’s necessary to eat 5000 calories for 5 days. That can’t be easy. And if the quantity required is. different for a man or woman
Also what about sample high-fat menus that get the number of fat grams up sufficiently ?
Take a look at Dave Feldman’s website to get more specific info.
So, please put all this wonderful information into a keto program for weight loss and keeping cholesterol numbers good.
Great article. I love Dave Feldman’s work. His presentation provides some amazing information about energy homeostasis. I especially love how the Liver ‘relaxes’ when there’s enough fat. The statin companies better save their money for the class actions that are sure to come. Thanks for this article. Wonderful.
Article comparing lipids in “fasted” and “fed” polar bears
http://www.docsdrive.com/pdfs/ansinet/pjn/2002/73-78.pdf
The Essential Fatty Acids and the Diet of Polar Bears (2002).
Nice link. Thanks.
Dr. Mike:
Really like your blog.
My GP has given up mentioning statins, after I laughed at him.
I suspect there is a big note in my file stating “Patient refuses meds”.
Any suggestions on how much (grams) fat to eat per day?
(I am female, 64 years old, just started on LCHF diet.)
Thanks!
Kitti
“… people say, Oh, you’re on one of those crazy low-carb diets”
I take your point that it makes no sense for people to make this remark when even by their standards you’re eating less fat (and less refined carb) by removing/foregoing some of the total, but what’s really in their mind is that this is indicative of a general approach that worries them – if you’re doing that then you’re probably not getting “Plenty of healthy [sic] whole grains and fiber” as they have learned by rote that one must do. You won’t be eating your muesli for breakfast and having pasta salad for dinner and so on. They might even suspect you of not cutting the fat off your steak!
“what’s really in their mind is that this is indicative of a general approach that worries them –” – This is exactly what happens to me as well – we have an RD in the family who is absolutely convinced that I am going to keel over any day now. Not even my excellent bloodwork at my most recent (May 2017) physical has put a stop to her endless rants about fiber (no thanks – I read “Fiber Menace” and it made SO much sense), whole grains (no thanks – I read “Wheat Belly” and it, too made so much sense), and “all that fat!!” (cue dramatic, Sarah Bernhardt-worthy hand-to-forehead pose). I have also explained to her, ad nauseam, that I just feel so much better and am happier (and have lost a few pounds that needed to go). All with very little effort and deprivation (I have no willpower in the face of true hunger, which was what I had for so many years before reading “Always Hungry?”). Meanwhile, she is absolutely mystified as to why I do not want to join her in her food choices. You know, because being 40 pounds overweight (and still going up), being on a statin for her high cholesterol, being on a blood pressure med for her HBP, and probably (in my estimation) being either an unconfessed, or an undiagnosed diabetic is all working out so well for her. She doesn’t get why *I* am mystified by her choices! Seriously!?
Oh she must be related to one of our doctors, who told me sternly that “everyone has to eat lots of carbs or you will have no energy” and that “diabetes is always progressive, it’s the nature of the disease”.
Strange that because I’ve spent about twelve years now eating around 50g carbs/day, mostly not from grains, and I have lots of energy from all the fats and ketones I metabolise, in fact I spend most of my time metabolising stored energy from the previous day’s meal – or sometimes two smaller meals – with just a snack sized breakfast. Also I was so “prediabetic” that it made little difference and now my BG is so normal that I stopped bothering to test. Only 5mg Amlodipine for mild hypertension and Carbimazole for hyperthyroid (a recent development). No more statins, H2 blockers or antidepressants either, and I soon lost all the weight the dietician and her infernal low fat diet made me gain.
Meanwhile she had so much energy she ran out of places to store it – she was the size of a bungalow and recently became prediabetic if not completely diabetic herself.
Couldn’t give up her Holy Health Grains though, she turned to 5:2 fasting and has finally lost some weight. Yet I am the one in danger . . .
I attended a Sally Fallon talk 14 years ago. She indicated to eat high fat meals without fasting before your next blood test to avoid being labelled a CVD risk by your insurance company. This was before Obamacare, of course.
Great work Dave is doing. Didn’t know you were once an Engineer. There are a few other (former) Engineers like Dr. Bernstien, Ivor Cummins thefatemeror.com, etc. who are doing well for the LC community. Keep up the good work.
The kind of experiment discussed here shows the value of n=1 to n=10 experiments by intelligent people as compared to n=10000 trials by idiots with blinders on.
Nicely put!
Yes Dave’s work is brilliant, and I can tell this in three ways
1) his work is brilliant
2) he has discovered something to my reckoning previously unknown to science – or if it WAS known it has been steadfastly ignored – which has punched a huge hole through current dogma and demonstrated something that is important enough to require further research
3) the desperation and vehemence of the attacks on him by Conventional Wisdom Trolls who have even appealed to Ethics Committees to stop him continuing to research even on himself
Thanks, that is truly amazing work! I know you’re busy but if you get a chance please let us know what you think of this (podcast): https://chrismasterjohnphd.com/2017/07/22/biochemistry-insulin-doesnt-make-fat/
I haven’t listened to it, so I can’t really comment.
Hi Dr. Mike,
I’ve been a Protein Power practitioner since the beginning and love your posts. These recent ones on cholesterol are so timely and important. All the info above and emails reflect my experience, so I don’t need to go on and on. The new part is to eat fat before labs which I will do next time. Another sane voice on cholesterol is Dr. Malcom Kendrick, a Scotish physician, who has a Blog and authored The Great Cholesterol Con. I recommend it. Thank you for your life saving work, Dr. Mike.
This is one of the most informative pieces I have ever seen. My doctor has not wanted me to go on a ketogenic diet, but I have tried to control borderline diabetes by eating a low-calorie diet, on the the theory that the insulin drives a cascade of metabolic effects that include insulin resistance. (I used to be a carbohydrate addict.) Sometimes it is hard to avoid refined carbs since I live in a monastery and not every meal is user friendly. Still, I generally eat what is pretty much a SAD minus bread, potatoes, pasta, and rice. My lipid panel generally has reflected dietary discipline, but not always. The time before last it was out of whack. So before my last test I made a point of including more lips (mainly from butter, cheese, lard, and olive oil) in my diet. The figures improved in my last test. Now I think I will be safer if I track the weight of grams of fat to make sure I get what I need.
Typo in what I just wrote. Instead of low-calorie diet, I should have written low-carbohydrate diet. It would be useful if the website would let you edit a comment if something like this turns up.
Very interesting and informative presentation!
My wife and I started a grain free, no sugar diet about 2 months ago. It wasn’t a big transition as we had started moving in this direction a couple of years ago. The main incentive to go ketogenic was to deal with my wife’s worsening arthritis that required increasing reliance on pain killers. It seemed logical that a ketogenic diet would benefit me as well. We eat locally produced organic produce, free range beef, organically raised chicken and eggs, etc., plus what we can grow for ourselves in our backyard organic garden.
Fifteen years ago I landed in the hospital with angina which lead to stents and the beginning of the usual drug protocol for heart disease. At the time my cholesterol levels from several tests averaged roughly 150 mg/dl (3.9 mmol/L) total cholesterol, 75 mg/dl (1.95 mmol/L) LDL, 58 mg/dl (1.5 mmol/L) HDL and triglycerides ranging 65-90 mg/d/ (1.68-2.33 mmol/l). Clearly on the low side and somewhat contradicting the lipid hypothesis for heart disease.
Changes to my diet over the ensuing years resulted in my cholesterol numbers slowly increasing, although with good numbers. I was also lucky to be able to stop taking most of the heart meds except for blood pressure meds and daily aspirin. Much to my dismay however, my GP prescribed 20mg of Crestor when I turned 60. I decided not to take the statin (unknown by my doctor) and managed to improve my cholesterol numbers through diet. Out of the blue last fall, my GP decided that I needed to increase the Crestor to 40 mg as new guidelines deemed that LDL levels need to be kept under 78 mg/dl (2.0 mmol/l).
I resisted the temptation to start taking the drug (again unknown by my doctor) and this was about the time that my wife and I started to move to a ketogenic diet. My cholesterol numbers moved higher as a result with total cholesterol at 214 mg/dl (5.53 mmol/L), LDL at 106 mg/dl (2.75 mmol/L), HDL at 98 mg/dl (2.54 mmol/L) and triglycerides at 20 mg/dl (0.53 mmol/L). Three months later and 6 weeks into the full ketogenic diet my cholesterol numbers climbed enough to have my doctor foaming at the mouth to increase my cholesterol meds, this time adding 20 mg ezetimibe to the 40mg of crestor. This most recent test had total cholesterol at 240 mg/dl (6.24 mmol/L), LDL at 117 mg/dl (3.03 mmol/L), HDL at 119 mg/dl (3.08 mmol/L) and triglycerides at 11 mg/dl (0.29 mmol/L). My HDL/total cholesterol ratio is 0.49 (double the ideal level of above 24%) and my triglyceride/HDL ratio is 0.094 (way below the recommended level of under 2). I should add that the LDL numbers are ‘calculated’ and it would be very difficult for me to have direct measurements done in my part of the world.
Given that my triglycerides have stayed in the 10-20 mg/dl (0.26- 0.65 mmol/L) for years, it is doubtful that my LDL levels contain significant amounts of small particle sdLDL. Even with my history of heart problems, I just don’t see the benefit in taking statins given the potential side effects of long term use.
Btw, my wife was able to stop taking pain medications for her arthritis after a couple of weeks into the ketogenic diet.
Thanks for the history. I see this kind of thing all the time.
Paul — your numbers are unbelievably stellar! I now have people sending me their labs constantly and I rarely see a pattern such as yours. In fact, I don’t know that I’ve ever seen a delta between HDL and TG like this, even in the most athletic hyper-responders (where it is most likely).
This has been a question that has been constantly on my mind… where do my cholesterol results fit in with the general population. I have done considerable online research on cholesterol over the past year, especially in light of my evolving numbers resulting from my move to a paleo/ketogenic diet. I have been scouring the net trying to find relevant comparisons with other people but, up until now, has been an exercise in futility. I was fairly confident that my numbers were good, if not excellent, but the small increase in my LDL values has been a bone of contention with my GP.
Overall, it is my firm belief that if the population as a whole woke up and adopted an unprocessed, organically sourced, whole foods ketogenic diet, that the vast majority of these people would see their lipid profiles improve dramatically, as well as resolve many chronic health issues.
My data is not very different from Paul:
CT 312
HDL 139
LDL 165
TG 40
It’s good, okay?
You make a comment above that I find a little confusing.
“I suspect they reflect the low-fat, low-calorie nature of my regular #LCHF diet. ”
I read LCHF as ‘low carb hight fat’ which is not what the extract above seems to suggest or have I completely misunderstood your point.
What I was trying to get across is that a low-carb diet (#LCHF) can be a low-calorie diet as well.
I wonder if what might be critical in some of the results Feldman is claiming is whether saturation dynamics is being triggered. Any ingestion of fats which doesn’t achieve saturation level might result in a linear relationship between fat ingestion and subsequent measurement of lipids. Saturation dynamics may be totally different. I would think that probably lots of experiments have been done with fat loading and subsequent lipid levels, including varying the types of fats consumed. I imagine that ordinarily a linear relationship is demonstrated. I only have a layperson’s science background so these are speculations.
All of this new information is very thought provoking, but I don’t know whether “to play” with this myself or not, out of concern that I’d get a mega cholesterol and megal LDL reading. Also, at present I haven’t been consistently low carb anyway. Ironically though, the very day this blog post was published I had just come home from a (depressing!) “statin talk” sandwiched in unexpectedly during a physician’s visit for something else. It was low key because my physician is in the “exercise and eat nothing white except oatmeal camp” and always adds “but statins have their problems.” However, he did firmly say, “with your LDL you probably should be on a statin.” [TC 239, Tri 92 (up from 70 in past ?), HDL 65, VLDL 18, LDL 156].
This is a really interesting article and it raises a question. My family doctor absolutely insists that I take my cholesterol tests non fasting. When I go to the lab to take my blood, they give me a hard time because I have not fasted for the requisite 12 hours, despite the fact this is how the doctor ordered my test. If eating high fat 3 to 5 days before a test can affect cholesterol numbers, I assume taking the test non fasting has some clinical value?
Don’t have any idea what your doc’s motivation or rationale is.
Maybe trying to catch him out? I suspect that was my doctor’s motivation in having me do an unfasted test – she wanted to see how much worse my postprandial lipids got. I think she was surprised that they were almost identical to the fasted ones, in fact I can no longer remember which were the unfasted results. I suspect unlikely to happen on a high carb diet.
I just reviewed my test results, as a non-hyperresponder – the statin reliably dropped my LDL but had little effect on anything else. Going hyperthyroid had almost exactly the same effect. Going LCHF doubled my HDL and dropped my trigs to 1/10 of what they were. Either adding more saturated fat or stopping losing weight caused a minor change where my HDL went up and my LDL down by about the same amount. Other changes to HDL and LDL over the years are basically noise, and changes in trigs slightly noisier noise.
So like the swan sailing serenely along it looks like nothing much is happening, but Dave has revealed all the paddling going on under the waterline. Who knew the system was actually so dynamic?
With trigs consistently under 100 and HDL over 50, my now unmedicated LDL is around 150 and at my age I suspect this is probably exactly where I need it for maximal benefits. Gotta transport that fat around so I can metabolise it.
Hi Dr. Eades!
I went onto a ketogenic diet a couple of weeks ago (started off more liberal, gradually working to a more strict lifestyle – has helped with not suffering ‘keto flu’ quite nicely!). Your blog is fascinating, and very encouraging.
So many problems even in two weeks have vanished: aches and pains, no PMS this month, no bloating, no head-fog and my muscles no longer feel like they can’t hold up my body. (I was, embarassingly, on a complete junk-food diet before this for several years)
Keep up the great work – statins are EVIL. My dad was on them, and instead of dying of the heart failure he had, he died of kidney and liver failure due to medication and the recommendation of ‘eat less fat’.
I’m surprised no one seems to have asked this: I don’t need to tell you that there’s been a lot discussion about a substantial percentage of LCHF’ers who are supposedly “hyper-responders” to saturated fat, with their cholesterol numbers dramatically elevated because of it. It’s been often suggested that those people might want to switch their fats to those with a high fraction of monounsaturated fats, instead of saturated, and perhaps even add carbs to break out of ketosis. I’m not sure that there’s any science yet to suggest that it’s dangerous to have your cholesterol kicked up this way, but in light of your article it does raise the question as to whether those individuals could get the effect that Dave Feldman is publicizing–since in Dave’s scenario it seems to be that vastly INCREASING the intake of saturated fat (at least for a few days) would normally result in the cholesterol being lowered, not raised. Any comments? It’s perplexing!
I don’t know for sure the answer to your question. But, if you listen carefully to Dave’s presentation you’ll notice that he mentions that a number of people crank up their fat intake by eating Macadamia nuts. The fat in Macadamia nuts is primarily monounsaturated fat. There is about five times more monounsaturated fat in these nuts then there is saturated fat. Since the folks who used these nuts to increase their fat intake had their cholesterol levels fall, I would assume monounsaturated fats would work well, too. As to whether it would work as well, better than, or worse than saturated fat, I’m not sure anyone knows. Would be an interesting subject to study.
This article made me laugh out loud with pleasure. I’ve had total cholesterol in the mid 300s for 30 years that I know of when I had my first cholesterol test. I’m still alive and well at 81.
Hey Dr Mike, interesting post as always. Have you experienced patients who undergone bariatric surgery for weight loss during your practice and still stayed on low carb after? I am contemplating sleeve gastroctomy and still researching data as far as long term success. Thanks!
Most of the ones who are successful do follow low-carb diets after surgery.
Thank you!
I am a hyper-responder who is now 79 years old. My total cholesterol was around 200 with a healthy conventional diet 15 years ago. My triglycerides were nearing 400. My testosterone level was 289 ng/dL and I started taking testosterone supplements. My doctor later prescribed Lopid to lower the triglycerides. I decided to go on an LCHF diet instead. This approach brought my TG down near 100, but my TC went up to around 350. I was on this regime for around 12 years when I decided to go off my testosterone supplement. The resulting testosterone level was a perfectly normal result of almost 700, which is quite a bit higher than President Trump’s 4xx. What to make of these results? I think the LCHF diet was what I needed to improve my general metabolism, statins be-damned. By the way, I fired a GP who tried to bully me into taking statins and found a more compliant physician.
I wanted to clarify my too-brief remarks above. I did not explain why I stopped taking testosterone supplements. I found a research article concerned with the testosterone levels of men with metabolic syndrome. These men presented with lower than average levels of testosterone. I did not have all the symptoms of metabolic syndrome, but my three siblings all developed diabetes. Because I had become normalized with the LCHF diet, I thought that my testosterone levels would also have become normalized. I was proved right. Low testosterone levels are often a sign that something has adversely affected the metabolic processes. Taking testosterone supplements will most likely not improve your metabolic processes. Likewise, taking a statin will most likely not improve your metabolic processes, even though you may then attain the cholesterol levels of your youth.
Good for you re firing a doc who tries to bully you.
F.A.O. George Smith and FH
Hi George
Just read your comments on FH and that high cholesterol (constantly in double figures e.g. 10 mmol/L here in England) plus xanthelasma is a good diagnosis of FH.
Would you know what the genetic test(s) would be, which you allude to?
I put FH into the search engine on Zoe Harcombe’s website and there was an article on FH….a gene defect on chromosome 19 if I read correctly. And she does mention a few times about getting a proper genetic test for the condition but no specifics.
I can see my xanthelasma, but I’m sure my blood tests over the years were fasting ones. In the context of this blog, the fasting may have pushed the levels up (and possibly constant stress over the years too).
Your comment indicated it was not straightforward experience for you but I would appreciate any guidance. As always, I anticipate maximum resistance if I go before my doctor with this sort of request.
Regards
The appliance of science would be useful to get definitive confirmation
Hi Dr. Eades,
Thanks for sharing this (and for the other useful information on your website). I had my cholesterol checked for my physical earlier this week. Total cholesterol 288, HDL 120, LDL 155, and tryglcyerides 67. Last time (3 years ago) these were 243, 95, 138, and 50, respectively. I am 65, 203 lbs. and 6’3″ in height. High cholesterol runs in my family. After years of my MD’s insistence, I went on statins for about three years. After reading Gary Taubes’ book, your website, and similar materials, I stopped the statins. I largely avoid starches and sugars (save for red wine!), eating leafy greens (a plate full) twice daily, plus other veggies, and protein at all meals (grass fed beef, etc.). I lift twice weekly and take one-two demanding walks per week (plus calisthenics). I feel great. My doc’s only expressed concern was the higher LDL number. My blood was drawn 36 hours after a four-day long weekend (and related over-indulgences), so that may have impacted the number.
Thanks again for sharing solid information and your wisdom.
Thanks for the in depth article Dr. Mike! Very informative. I am beginning my journey to lowering my cholesterol and found this just in time. Thanks a lot for sharing!
Hi Dr. Mike,
thanks for your great blog and this posting.
I have a question if you don’t mind. The text says:
“One of the problems with the high-carb, low-fat diet is that people following those diets tend to have their LDL-particle size get smaller, which is not a good thing. ”
I’ve no formal background in medicine but live carb free for a decade and read a lot. I so far did not come across any reference that LCHF diets tend to decrease the LDL-particle size. Sugar, no sports and for a share of people a genetic disposition are usually blamed as the cause for the increase in the share of small particles.
I’d appreciate if you could drop a clarifying note. Thanks much.
Andreas
I think you misread what I wrote. LCHF diets do not make particle size smaller – in general, LCHF diets make particle size increase. It is the low-fat, high-carb diet that makes the particles smaller, as I wrote in the lines you quoted above.
Dr. Mike,
you are right, I picked it up the wrong way and even when discussing with someone else we did not discover the we turned the message around. Thanks for clarification.
Andreas
what fat did you add? mac nuts are mono unsaturated but you mention saturated? I can see eating more hamburgers and butter……cheese? 450 grams fat and 194 grams protein…..where do you get 200 to 250 grams fat from? which fat is optimal? saturated?(eat butter cheese…?) mono?(drink olive oil) omega3(drink flax seed oil?)
I’m just tossing out a caveat that I tried the three day increased fat protocol by enormously increasing just my ordinary fat intake, while keeping carbs low, but not pushing my calories up to 5000 or so, which Feldman recommends. My total cholesterol and LDL both went up (239/266, 156/182), values about which my physician will probably now express alarm as opposed to his former mild admonishment. As Larry posted above, I couldn’t determine which foods to eat that kept carbs low (Feldman did 35 carbs/5000+ calories) and jacked up fats, but not saturated, unless I did literally drink olive oil. Cheese drags in carbs as would more nuts, and butter is saturated fat. Also, another variable in the protocol failure for me might have been that I wasn’t consistently low carb (40-50) for all the prior months, although typically I stayed between that and around 150.
Copying part of my message from up the top in case you missed it:
I eat high fat/low carb, have done for about ten years, but for a week before my lipid test last week I ate extra, extra high fat. My total cholesterol came down from 8.7 (336) to 5.5 (212), my HDL remained exactly the same at 3.5 (135), my triglycerides lowered from 0.5 (44) to 0.3 (26), and my LDL lowered from 5 (193) to 1.8 (69) !
I just added extra, extra coconut oil to my veggies and meat, plus ate a lot of fatty lamb, and ate macadamia nuts, almonds and full fat cheese for snacks inbetween meals. I eat paleo apart from the bit of cheese for snacks – it was tricky to work out how to get extra fat and the macadamia nuts are prety expensive so I compromised with a bit of cheese. I’m very lean and didn’t put on any weight despite the extra calories.
I can’t imagine what my endocrinologist, cardiologist and GP are going to say – I shall tell them I upped the fat content of my food as I was trying to put on weight.