Just read through the August issue of the American Journal of Clinical Nutrition, which was chocked full of good articles. I’ll be kept in blogging fodder for several days just from the contents of this one issue.
The paper I want to discuss today is one that I find hilarious. It’s a report of the Hamburg Burger Trial and I find it hilarious because the results were so different than what the researchers expected. In fact, they mention how surprised they were to get these results. The only reason they should have been surprised is that they are either ignorant or stupid – or both.
If I gave most readers of this blog the same data the authors of the study had, the blog readers would not have been surprised. They would have expected exactly the outcome that resulted. Which makes the readers of this blog a whole lot smarter than the long list of scientists who authored this paper.
Here’s the setup.
Researchers in Hamburg, Germany recruited 24 healthy subjects with an age range from 18 to 65 years of age. They had these subjects undergo a 12 hour, overnight fast then show up at the lab where they provided a blood sample then baseline vascular function testing. Two hours after all the testing, the subjects were given one of the following meals from a Hamburg McDonald’s to eat:
a conventional beef burger meal consisting of a 211-g beef burger (Big Mac; McDonald’s Corp, Oak Brook, IL) with 152 g French fries, 20 mL ketchup, and 500 mL carbonated lemon-flavored soda (Sprite; Coca-Cola Co, Atlanta, GA) (meal 1); a vegetarian burger meal with standard side orders consisting of a 203-g vegetarian burger (GemüseMac; McDonald’s Corp, Munich, Germany) with 152 g French fries, 20 mL ketchup, and 500 mL carbonated lemon-flavored soda (meal 2); and a vegetarian burger meal with vitamin-rich side orders consisting of a 203-g vegetarian burger, 90 g salad, 30 mL balsamic dressing, 306 g yogurt with fruit, and 500 mL orange juice with
200 mg vitamin C [Minute Maid; Minute Maid (a division of the Coca-Cola Co), Houston, TX] (meal 3).
Two hours after the subjects chowed down on one of these meals testing was repeated and repeated again four hours later.
The subjects went away and came back a week later and went through the whole rigmarole again until all 24 subjects had eaten all three of the above meals.
Before we get into how the results of the vascular function testing in these subjects came out, let’s digress a little to look at what was actually being tested. If you’re not interested in the how-tos of vascular testing, skip on down.
Arteries, the vessels that carry oxygenated and nutrient-rich blood to the tissues, are muscular tubes of varying size that have an inner lining that is incredibly complex in its action. This inner lining called the endothelium is only a single cell thick yet it controls the activity of the entire artery. The endothelium senses and responds to a multitude of both internal and external stimuli and produces and secretes a host of substances that can cause the artery to constrict, to dilate, and to repair itself. It can cause the blood to clot and can bring about interactions between various blood components. And this extremely powerful organ can’t even be seen with the naked eye because it is a layer one cell in thickness.
Since the endothelium is only a single cell in thickness it is prone to injury. In fact, most heart disease is caused by damage to the endothelial cells of the coronary arteries. Plaque forms beneath the endothelium and is usually initiated in an area of damage to the endothelial cells.
One of the ways scientists have developed to measure endothelial function is by what is called flow-mediated vasodilation (FMD).
When the flow of blood increases in an artery, the endothelium secretes substances that make the artery expand (dilate) to better carry the increased flow. When the endothelial cells are working properly they secrete plenty of whatever it takes to make the artery dilate; if the endothelium isn’t working or is inhibited by a drug or other substance or is injured, the cells don’t respond as well to the increased flow and the artery won’t dilate as much as it would were it under the control of a non-impaired endothelium.
Here’s how the FMD test works.
While your sitting comfortably and relaxed I use an ultrasound measuring device called a Doppler to determine the size of one of the arteries in your upper (or lower) arm. This procedure is painless and non-invasive. It’s much like getting an ultrasound test to see a developing fetus. Once I determine the size of the artery I put a blood pressure cuff on your arm and crank up the pressure. I get the pressure high enough to shut off blood flow in the artery I measured. I leave the cuff pumped up for a couple of minutes to let the blood in the artery beyond the cuff drain out and get carried away by the veins. Your arm beyond the cuff will start to turn kind of white due to this loss of blood in the tissues. Then I release the cuff. As I do the blood rushes in to fill the void. When it does it increases the flow through the artery in question. If the endothelium is healthy and is working properly it will quickly secrete vasodilating substances that will make the artery increase in size to accommodate the increased flow. If, on the other hand, the endothelium is damaged or is inhibited by a drug or other inhibitory substance in the blood, the endothelium won’t secrete the vasodilating substance quickly and the artery won’t dilate as much.
If I have a baseline reading of your FMD then give you an unknown drug and test again I can tell by how much your artery dilates after the drug as compared to how much it dilated before whether or not the drug is harmful to your endothelium.
The researchers conducting the Hamburg Burger Trial assumed that meal #1, the one containing the real McDonald’s hamburger crawling with saturated fat would knock the FMD test in the dirt and while meals #2 and #3 would show less endothelial damage because, after all, they were vegetarian and had almost none of that nasty saturated fat in them. Plus they had all these good antioxidants that the plain ol’ McDonald’s burger meal didn’t have.
Before I tell you the results, I want you to look at this chart that gives the macronutrient breakdown of the three meals.
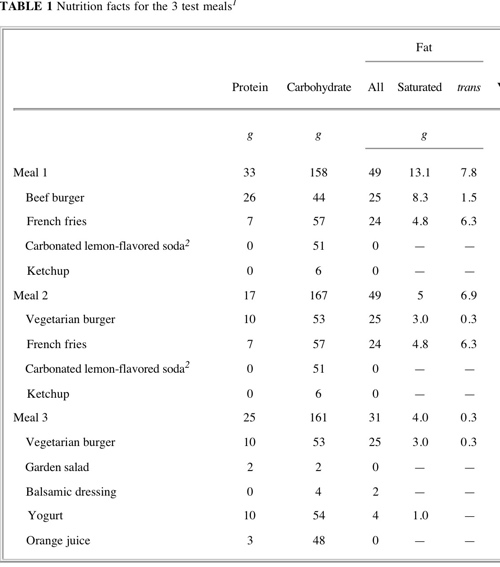
Despite differences in fat and saturated fat (which obviously were the only macronutrients these researchers figured would have an effect) note that the massive amount of carbohydrate is almost the same in all three meals. Knowing what you know about the physiological effect of carbohydrates, what would you expect the results of the FMD studies to be?
You are correct. The reduction in FMD was the same after all three meals.
The 160 or so grams of carb in these meals represents about 32 teaspoons of ‘sugar’ that has to be dealt with. Since a normal blood sugar is only one teaspoon of sugar dissolved in the blood, that means that these subjects had to dispose of 31 teaspoons of sugar fairly quickly. They did so by increasing their insulin levels, which drove the sugar into the cells, including the endothelial cells. In fact, the insulin hit the endothelial cells first because they line the arteries carrying the insulin through the body. And since insulin is a vasoactive hormone, one would expect a vascular reaction.
Plus, as I wrote before, eating is an inflammatory event just like breathing. We have to do both, but we pay the price. During inflammation the endothelial cells don’t function optimally. So getting rid of the huge load of carbohydrate and the accompanying inflammatory effect of the food (and, don’t forget, high glycemic carbs are the most inflammatory of all the macronutrients) inhibits the normal action of the endothelial cells. Anyone with half a brain and a rudimentary knowledge of the nutritional aspects of physiology would have predicted that the FMD would have declined about the same with all of these meals.
The only ones who didn’t realize this were the researchers who did this study. As they reported:
Against common expectations, a conventional beef burger meal and presumably healthier alternatives such as vegetarian burgers with or without vitamin-rich side orders did not differ significantly in their acute effects on vascular reactivity. [my italics]
Not against common expectations, but against the expectations of those steeped in the idea that fats in general and saturated fats in particular are bad while carbs are good.
What I find particularly satisfying about this study is that it provides ammunition to use against Dean Ornish and the rest of the knucklehead rabid low-fatters. For the last several years these guys have been parading around on the talk show and lecture circuit crowing that a single high-fat meal causes endothelial dysfunction based on a study (that I can’t lay my hands on right now because I’m in a hotel in Anaheim getting hurried to finish this up and take the grandkids to Disneyland (and believe me, I’d rather take a beating than spend the day at Disneyland, but, hey, I’m a doting grandfather)) showing that someone who ate a single hamburger meal had decreased FMD. I’ve countered by saying that it wasn’t the fat that caused the decreased FMD, but the overall meal and primarily the carbs. But I had no data to prove that until now.
I’m sure these folks in Hamburg figured that they would show that the ‘bad’ meal of a real beef burger would cause a substantial drop in FMD while the ‘good’ meals of veggie burgers would show a much lesser effect. Fooled them.
In the words of the old sixties song Where Have All the Flowers Gone
When will they ever learn, when will they e-e-ver learn.

Nothing wrong with a McD’s double cheeseburger if I just throw away the bun. On a recent road trip I had no food with me so that was my lunch–it had been a loooong time since I’d been to McDonald’s and it was surprisingly tasty.
I wouldn’t know. I haven’t had one in years.
Cheers–
MRE
I’ve tried to research this topic (ED) before. What I have been unable to figure out is how the researchers came to conclude that the changes noted in endothelium is indeed dysfunctional. Yes, I’ve read many a paper that demonstrates the phenomenon – what I’ve yet to find is their evidence that these changes are harmful or “dysfunctional” as opposed to a desired response to certain stimuli. I know many people are convinced that “endotheial dysfunction” is a precursor to CAD but I’m not so sure they are right.
Hi labrat–
I about half way agree with you. No one knows that FMD is the true measure of endothelial dysfunction. It’s just a test that seems to make sense, but, in my view at least, is far from optimal. I feel fairly certain, though, that real endothelial dysfunction is a precursor to coronary artery disease, which is the ultimate in endothelial dysfunction.
Cheers–
MRE
Wow! It’s the “McDonald’s Paradox” – sat-fat-containing burgers show no more endothelial damage than the healthy veg alternative. How could this be? Think, think, think…
I know! There must be some sort of chemical in the ketchup that counteracts the artery-clogging effect of the saturated fat!
😀
I’m sure they’re busy trying to concoct the ad hoc hypotheses at this very moment.
Cheers–
MRE
I actually wrote the above snarky “Mcdonald’s paradox” comment before clicking the link to the paper. After reading the abstract, I’m a little bit amazed.
The first sentence is disturbing in that an (incorrect?) assumption is stated is undisputed fact:
I’m not sure I understand the last sentence:
I hope I’m wrong, but I interpret this to mean something like, “well, we didn’t get the results we expected, so decline in FMD after meals must not be meaningful.
If so, these people really are bozos.
What about doing a followup study, comparing the effects of an almost-no-carb meal with an almost-all-carb meal?
-Dave
Hi Dave–
You’re right on all counts. In the first sentence the authors stated as true something that is unproven and controversial. They thought it was true, though, which is why they were so surprised at the results.
The last sentence I don’t really understand either, and it wasn’t elaborated on in the paper. I think it’s simply gives them a way out of the corner their data has painted them into.
Cheers–
MRE
Sir do you know the work of Nick Gonzalez MD ?
He trained at Sloan Kettering as i recall and has been doing his stuff for decades and he and Linda Isaacs have the most incredible remission rates for patients of stage 4 cancers; and the interesting thing is that although he sometimes uses a vegetarian diet any of his protocols use what ‘we’d’ call a paleo diet.
Have never actually heard him speak in person but here he is.
http://www.mandjshow.com/videos/alternative-medical-choices/
Don’t know him from Adam, but he sounds interesting. I’ll read more.
and i’d forgotten about his grant and though many try to tie him to Kelley when he came upon Kelley work as i recall he chucked oot owt that dubious in its case history
http://members.aol.com/pbchowka/gonzalez-cafta.html
What role do free radicals play in inflammation? It is my understanding that the antioxidants in fruits and vegetable are needed to deal with preventing free radicals from oxidizing. There for what role do fruits and vegetables play in preventing inflammation?
Hi Tom–
Fruits and vegetables do provide antioxidants, but these antioxidants outside of the fruits and vegetables, i.e., in supplement form, have never been shown to be helpful in increasing lifespan or preventing disease. No one knows if it is really the antioxidants or the specific combination of antioxidants or if it is a compound as of yet undiscovered that provides the benefit.
The role of free radicals in inflammation is immense and way beyond the scope of a simple answer to a comment. The issue deserves a long post sometime.
Cheers–
MRE
Dr. Mike, a nice find and discussion as usual. I’m surprised that there has not been the usual number of comments in response; but maybe that’s because it’s hard, really, to think of anything to say about these Hamburg, Germany researchers expect that they are indeed a bunch of “Dummkoepfer” (forgive me if my German is a little rusty). Or maybe everyone is on vacation at the beach this week.
So here is a somewhat OT matter I’ve been wondering about: for a person who has been lo-carbing for awhile and in the process of losing visceral as well as subcutaneous (sp?) fat, which does the body shed first….the visceral stuff (like around the organs) or the other? Or does it tend to all happen more or less contemporaneously? And is there a practical way to figure out if / when you’ve reached optimal fat loss?
Best,
W
Hi Wil–
There are more comments, I just haven’t had the chance to get to them until now.
One definitely loses the visceral fat first. That’s the good news/bad news situation: visceral fat is unhealthy, but it comes off fairly quickly. To determine optimal fat loss, you can use the tables in Protein Power.
Cheers–
MRE
Dr. Mike, I wonder if you care to comment on a recently published study that reinforces statin-worship. It seems to contradict previous studies that identify risks associated with low cholesterol. Thanks.
Leeper NJ, Ardehali R, deGoma EM, Heidenreich PA. Statin use in patients with extremely low low-density lipoprotein levels is associated with improved survival. Circulation 2007; 116:613-618.
Hi Marilyn–
I read the study, which is meaningless. It’s an observational study, a kind of study that really has no value except as a generator of hypotheses. If I simply look at people who, for whatever reason, are taking a drug and compare them to people who aren’t, and find that those taking the drug have some change in condition that those not taking the drug don’t have, the info is meaningless. These studies – called observational studies – generate data that makes researchers say, hmm, that’s interesting. Maybe we should study it. Then subjects are selected who are then randomized to either a study group, which is given the drug, or a control group, which is given placebo. Neither the subjects nor the researchers know who got what until the study is over, i.e., it is double blinded and placebo controlled. Then if there is a significant difference in outcome, you have something.
Far too many people, including those who know better, try to make observational studies comparable to real, double-blind, placebo-controlled studies.
Hope this helps.
MRE
This is an interesting and related thing from the BBC –
http://news.bbc.co.uk/1/hi/health/6933799.stm
Obese ‘under-report’ sugar intake
Obese people underestimate the amount of sugar they eat, making studies into the condition based on self-reporting very unreliable, UK researchers say.
But a new urine test has been developed which can for the first time work out how much sugar people have consumed.
In a study of hundreds of volunteers, researchers compared what people said they ate with data from urine tests.
The findings appear in the journal Cancer Epidemiology, Biomarkers and Prevention.
“These results show what many have suspected for some time: obese people are not able to tell us what they actually eat,” said Professor Sheila Bingham who led the team from the Medical Research Council and University of Cambridge.
“If we are to tackle the scourge of obesity, both exercise and diet need to be taken into account.”
Linked after all?
Studies have suggested that eating more sugar is not linked to obesity.
But the report says these conclusion were based on studies which relied on self-reporting and that their findings show these to be inaccurate.
“The spot urine and blood tests established that obese people consume more sugar and less Vitamin C than their thinner counterparts, but this did not show up when asked,” said Professor Bingham.
“Although obese people may have a less active lifestyle than people of normal weight, reports about what they ate were less accurate than those from their normal weight counterparts.”
Dr Colin Waine of the National Obesity Forum said the tendency to under-report food intake among the overweight was a major problem for medical practitioners.
“Used sensitively, this test could be a great tool in helping patient and practitioner work out what’s going wrong and talk through what could be done about it.”
What a pity they did not test the burger on its own then as they had all the guinea pigs lined up and ready to eat as instructed.
Or do you know of a similar study where things with hi satd fat and lo carb/ hi carb content were tested in the same way? What was the outcome of that?
I don’t know of any such study, but I’ll stay on the lookout for one.
Cheers–
MRE
Haven’t diabetics been able to test for sugar in urine for like, ever?
For many, many years.
Dr. Mike
Outstanding post. I think I’ll steer tomorrow’s lunchroom conversation over to diet theory and then — between beefy bites of my green chili cheeseburger — I’ll enlighten my co-workers about endothelium health as it relates to saturated fat. I’m sure to impress and with some luck I just might convince one of the low-fatters at the table to eat sensibly again like our ancestors used to do. They had cheeseburgers way back when didn’t they?
Hello James–
Knowing your co-workers as I do, I would love to be a fly on the wall during this lunchroom discussion.
Cheers–
Mike
hi i enjoyed the read
You might be interested that AOL has a teaser headline/link today (8/21/07) that references the hamburger study. The story doesn’t provide many details, and the reporter’s conclusion is that all fast food is dangerous! Didn’t even consider that it was the carbs. Here’s the link: http://www.thatsfit.com/2007/08/16/healthy-fast-food-is-bad-for-your-heart-too/
Cathy